Malaysia might be first in the world to revolutionise pap smears in clinics

- 1.6KShares
- Facebook1.5K
- Twitter11
- LinkedIn14
- Email21
- WhatsApp65
Before we go on, let’s get a show of hands from all our female readers here…
Ask some women around you if they’ve done a pap smear and most would probably tell you that they’re hesitant about getting one, which is not far from what the Ministry of Health (MOH) reports indicate. These reports claim that an average of only 25% of eligible women got pap smears between 2013 and 2017.
Eh, why so low? Well for starters, pap smears are pretty unpleasant. Think spreading your legs for the gynae to shine a light up your hoohaa while inserting various objects (read: cold, metal, clampy) up said hoohaa. With that said, the low number could very well be due to the fear of getting hurt or being misjudged for promiscuity, or according to a survey by Jo’s Cervical Cancer Trust, embarrassment about the look and smell of their private parts.
“I worried about the nurse being able to take one look at my bits and have some magic skill to be able to determine the number of sexual partners I’d had. I thought a lot about what kind of underwear and clothes to wear.” – said a woman quoted by BBC.
Or even the uncertainty of what’s to happen during a pap smear.
“The mere thought of a Pap smear can be enough to bring on sudden anxiety, especially the first time around. When you’re a first-timer, the scariest part of all is not knowing exactly what you have to be scared about. Will it hurt? How big is the stick? They put it where? Exactly when does the whole ‘smear’ part occur?” – Kristie Mercer of The Thinkergirls wrote to news.com.au
This might have been the reality many Malaysian women face too. They could be your mom, guardian, sister, aunt, cousin, daughter, grandmother, wife, girlfriend, friend, and so on.
While it’s not easy for any woman to go get herself examined by a gynae, not knowing whether she’s one of the 3 out of 4 people who have deadly issues such as cervical cancer could be worse. It is sad considering that most women tend to underestimate their risk of getting something as deadly as cervical cancer, despite it being the 3rd most common cancer in Malaysian women!
But it doesn’t have to be like that anymore, because of this new CONCEPT of detecting cervical cancer in its earliest stages through a private initiative between University of Malaya (UM) and VCS Foundation Australia (VCSF) called ROSE (Removing Obstacles to Cervical Screening).
This project actually makes Malaysia a pioneer in innovating cervical cancer solutions
UM and VCSF worked together to create ROSE to, as its name suggests, remove obstacles to cervical screening. But before we talk about ROSE, first…
Not many people would be familiar with how pap smears work, so to further explain, here’s how it goes. According to WebMD, you’ll lie on a table in the doctor’s office and spread your legs while placing your feet on stirrups (or maybe even just on the bed). The doctor shines a light up the vagina for a clear, unobstructed view, before inserting insert a cold, metal thing called a speculum into your vagina.
The doctor then opens the speculum to widen the vagina, so that the cervix can be seen. Then, a swab (or a brush, like in the diagram below) is used to take a sample of cells from your cervix and then place them into a liquid substance in a small jar to send to the lab.
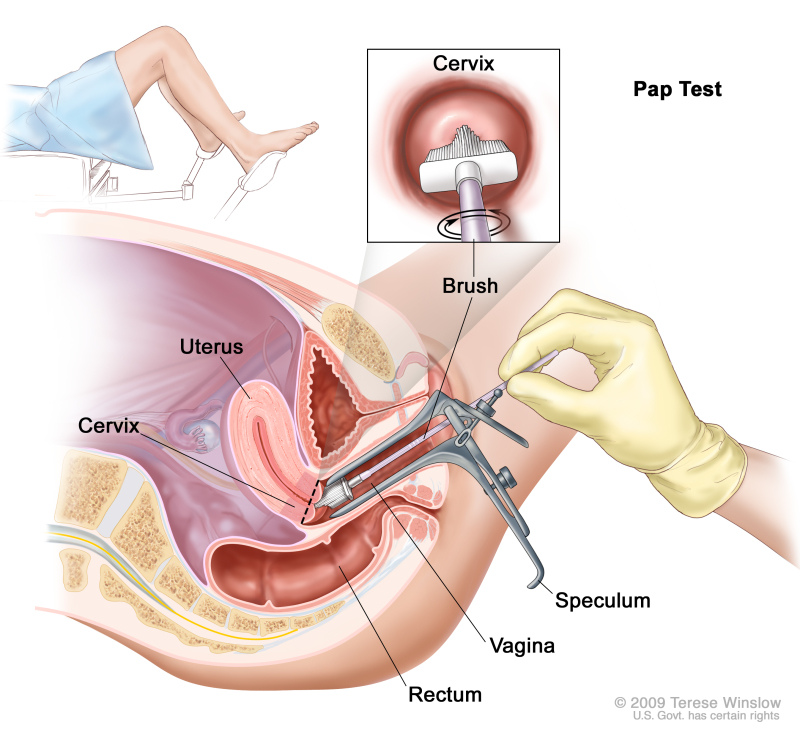
This procedure is one of the things that ROSE is trying to provide an alternative to, cause like we mentioned previously, it’s a very intrusive experience and can be really uncomfortable for the woman. So, instead of going through the unpleasant procedure of the pap smear, you can get a swab (which looks like an enlarged Q-tip) from the nurse or doctor at a selected clinic and do the test yourself using the instructions given.
Then, you return the swab to them for diagnosis and they’ll send you the results via SMS within 3 working days. This test which uses a swab is known as a HPV (HumanPapillomavirus) test, which tests for abnormal cervical cells, and this abnormality leads to cervical cancer if not treated soon enough.
HPV is commonly transmitted via skin-to-skin contact with a person who has HPV besides sexual contact, although it’s not clear how the HPV holding person got HPV in the first place.
There are many types of HPV and, although most HPV infections don’t cause much harm, certain types of HPV can lead to cancer, including cervical cancer. As we’ll tell you later, HPV infection and cervical cancer are at opposite ends of the time frame of cervical cancer development.

According to Professor Dr Woo Yin Ling, a Consultant O&G at UM whose role is influential in this programme, ROSE brings together self-sampling, HPV testing and an e-health platform (backed by VCSF’s population health management tool canSCREEN®).
“At its heart, ROSE is driven by empathy for the screening experience of women. It embodies safety, privacy and dignity through self-sampling, encouraging more women to willingly participate in screening in a timely manner.” – said Professor Woo.
Surprisingly, Malaysia is said to be the first country in the world to plan an integrated programme like ROSE. When we asked the program manager of ROSE Liyann Ooi about this, she told us that the e-health platform is integrated with mobile tech to help women register and receive results, and follow up all through a phone app.
“This mobile interface and its integration was specially designed for the Malaysian community and successfully demonstrated by ROSE as a well-accepted and feasible means of communication with the women to support them through their whole journey of maintaining good cervical health.” – Liyann Ooi told CILISOS.
And because every info is recorded and monitored, the clinics don’t have to look through their stacks of paper to see if must follow-up or not, or to do manual paperwork. So it’s quick and convenient lor.

Although we have yet to see the actual outcome of the ROSE concept, Professor Woo highlighted that a test run called the ROSE Pilot Project was conducted in 5 klinik kesihatans in 2018 to test and study the best ways to improve cervical cancer management in Malaysia.
She said that the project found that, out of the 4,188 participants, 5% of them tested positive and 3 cases of cancer were diagnosed and followed up on with the help of the e-health platform.
The study also found that healthcare professionals are also more likely to engage with the ROSE model because they know that more women would wanna get screened under ROSE and, like we said earlier, the staff no need to do so much paperwork since the e-health platform already helps with data collection and monitoring.
“The results confirm that ROSE is the right solution for strengthening our national cervical cancer screening programme.” – Professor Woo concludes.
There’s a very good reason why many women underestimate cervical cancer
Let’s first look at how cervical cancer develops. Similar to other cancers, cervical cancer takes a long time to develop. Young girls and women aged under 30 years old are usually just vulnerable to HPV infections, which is the very first stage.
And HPV infections can lead to abnormal pre-cancer cells in the cervix, which takes about 5-10 years for it to worsen to a high-grade abnormality. Then, 10-20 years after that, it can worsen to cervical cancer.
That’s why, for those under 30, HPV vaccinations are given to prevent the HPV infection from happening at all, while those above 30 have to go get screened to spot for abnormality and get treated before it gets worse.
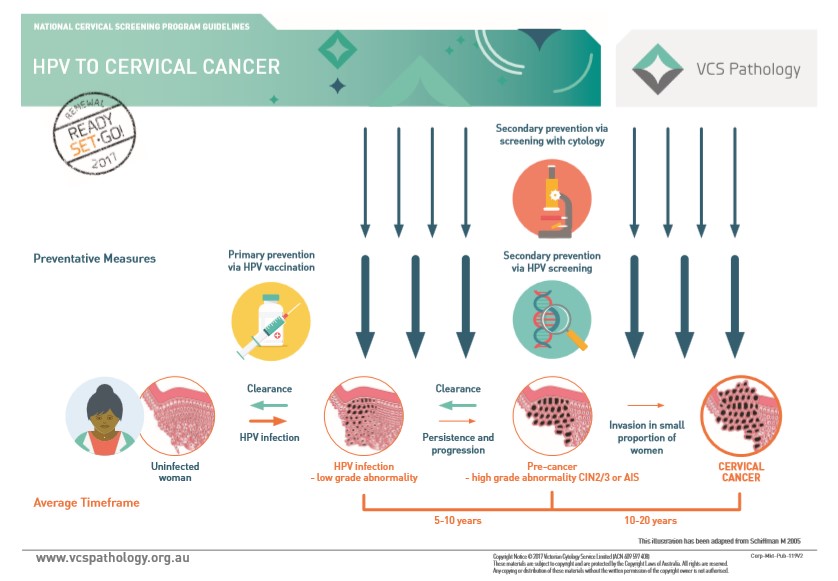
According to the Director General of WHO, Dr Tedros Ghebreyesus, Malaysia’s coverage for 13 year old girls stands at over 95%, thanks to the HPV vaccinations they started giving to Form 1 girls in 2010. And according to National HPV Vaccination Program Register of Australia, there are more than 40 types of HPV that can affect the genital area, but 9 of them are known to cause the majority of HPV-related cancer and diseases.
Used commonly and globally (including Malaysia), a vaccine called the Gardasil 9 activates the immune system to produce antibodies against the 9 HPV types. Hence, it provides protection against 93% cervical cancers, higher than the older vaccine which protected against 70% of them.
Apart from protecting against cervical cancer in females, this vaccine also protects against vulvar and vaginal cancer in females, penile cancer in males as well as anal cancer, genital warts and throat cancer in both.
So after understanding the best ways to manage cervical cancer, could this be the one?
Dr Tedros said that Malaysia is well on its way to meeting WHO’s target of screening and managing 70% of women aged 35-45 by the year 2030. He also said other targets include vaccinating 90% of girls by age 15 and reducing deaths from cervical cancer by 30%.
Maybe with this innovation, women in Malaysia don’t have to feel takut or malu about screening anymore. We probably wouldn’t have to see MOH reports quoting low percentages of cervical screening since the number of women who get screened would increase.
Thanks to this new concept, cases of abnormalities can be detected in more women, and more women can be saved before their abnormal cells become cancer. Along with the vaccination of young women, ROSE could be a huge first step towards eliminating cervical cancer in Malaysia. But to actually know how huge of a step, perhaps we shall wait and see…
And just to be clear, this programme is not in place yet, since it’s just the CONCEPT that’s been launched and NOT the programme itself. But if you want to get your hands on it, we hope that you’re okay with waiting for any official news regarding ROSE.
- 1.6KShares
- Facebook1.5K
- Twitter11
- LinkedIn14
- Email21
- WhatsApp65




